Phlebitis is a medical term that describes the inflammation of a vein. While the word itself might sound simple, the condition can range from a minor, localized annoyance to a life-threatening medical emergency. Inflammation causes the vein walls to swell, which can impede blood flow and lead to significant discomfort in the legs or arms.
At Vanishing Veins, our clinical approach begins with understanding that phlebitis is often a symptom of an underlying vascular issue. Whether you are dealing with a red, itchy patch on your skin or deep, aching pain that prevents you from walking comfortably, understanding the “why” behind your symptoms is the first step toward recovery.
Superficial vs. Deep Vein Phlebitis: Knowing the Difference
Not all vein inflammation is created equal. Medical professionals categorize phlebitis based on which “layer” of the venous system is affected.
1. Superficial Phlebitis (SVP)
Superficial phlebitis affects the veins near the surface of the skin. This is the type most people experience after a hospital stay or a minor injury. Because these veins do not carry the bulk of the blood back to the heart, SVP is generally considered less dangerous; though it is still incredibly painful. You may notice a “cord-like” feeling under the skin where the vein has hardened due to inflammation.
2. Deep Vein Thrombosis (DVT)
When phlebitis occurs in the deep veins, the large vessels buried deep within your muscle tissue, it is a far more serious matter. This is often associated with Deep Vein Thrombosis (DVT). In this scenario, the inflammation is accompanied by a blood clot (thrombus).
The Critical Risk: If a deep vein clot dislodges, it can travel through the bloodstream to the lungs, causing a pulmonary embolism (PE), or to the brain, potentially causing a stroke. These are medical emergencies that require immediate intervention.
What Triggers Phlebitis? Common Causes and Risk Factors
Phlebitis rarely happens in a vacuum. It is usually triggered by a specific event or a pre-existing condition.
Medical Interventions and Trauma
The most common cause of superficial phlebitis is localized trauma to the vein wall. This frequently happens in clinical settings via:
- IV Catheters: Long-term or improperly placed intravenous lines can irritate the delicate lining of the vein.
- Chemical Irritation: Certain medications delivered via IV can be caustic to the vein walls.
The Role of Varicose Veins
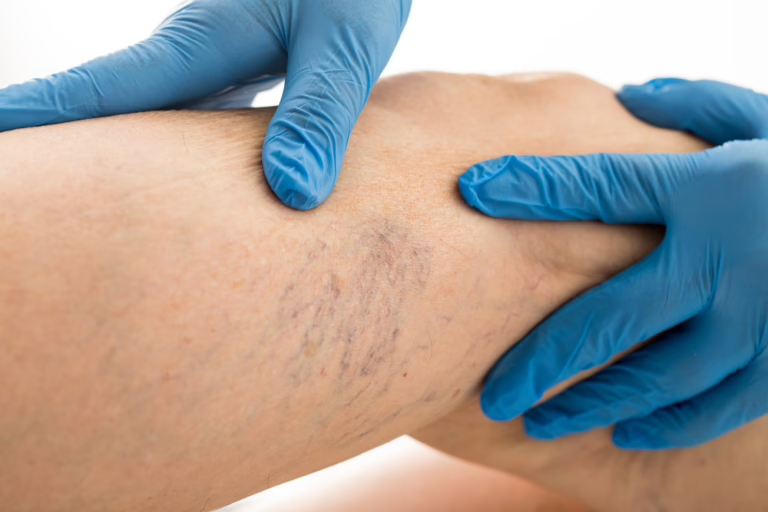
If you have visible, bulging varicose veins, your risk for phlebitis increases significantly. Varicose veins are caused by weakened valves that allow blood to pool. This stagnant blood is prone to inflammation and clotting. Our vein specialist in Tolland specializes in treating these underlying varicose conditions to prevent phlebitis from recurring.
Inactivity and “Economy Class Syndrome”
Your leg muscles act as a secondary pump for your circulatory system. When you move, your muscles squeeze the veins, pushing blood back up toward your heart. When you are inactive for long periods, the blood “stagnates”. As the blood sits still, it begins to thicken and clot.
Genetic and Lifestyle Factors
- Obesity: Excess weight puts localized pressure on the pelvic veins and slows down circulation.
- Pregnancy: An enlarged uterus can compress pelvic veins, while hormonal changes increase the blood’s natural tendency to clot.
- Cancer and Blood Disorders: Certain malignancies and treatments alter the chemistry of the blood, making it “stickier.”
Recognizing the Red Flags: Symptoms to Watch For
Phlebitis symptoms often creep up slowly, but they can intensify rapidly. At Vanishing Veins, we encourage patients to monitor for the following:
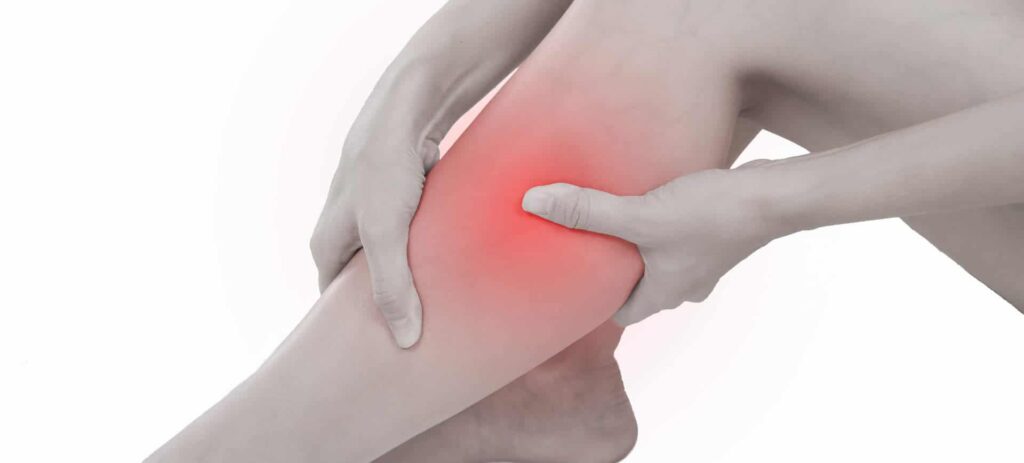
- Localized Redness and Warmth: The skin over the vein may look angry, red, and feel hot to the touch.
- Tenderness and Swelling: The affected limb may feel heavy or tight. Swelling often starts at the ankle and moves up.
- Burning and Itching: As the skin stretches over the inflamed area, it can become incredibly itchy.
- Morning Discomfort: Many patients report that pain is most pronounced first thing in the morning when they first stand up, as gravity suddenly increases the pressure in the inflamed veins.
- Systemic Symptoms: In severe cases, you may develop a low-grade fever or notice the skin over the vein beginning to break down or ulcerate.
Expert Diagnosis and Treatment at Vanishing Veins
When you visit Vanishing Veins, you aren’t just getting a prescription; you are getting a complete vascular evaluation with our vein specialist in Glastonbury. We utilize state-of-the-art diagnostic tools to determine if your phlebitis is superficial or if there is a hidden DVT that requires aggressive management.
Personalized Treatment Pathways
Depending on the severity of your condition, our experts may recommend:
- Topical and Oral Anti-Inflammatories: To reduce pain and swelling in superficial cases.
- Compression Therapy: Specialized medical-grade stockings that help move blood out of the affected area.
- Vascular Mapping: High-resolution ultrasound to check for clots and assess the health of your vein valves.
- Minimally Invasive Procedures: If varicose veins are the root cause, we offer modern treatments like endovenous laser therapy or sclerotherapy to “shut down” the problematic veins and reroute blood to healthier vessels.
Why Choose Vanishing Veins for Your Vascular Health?
Your veins are the highways of your body. When there is a “roadblock” like phlebitis, you need a specialist who understands the complex map of your circulatory system.
Our Expertise:
- Board-Certified Specialists: Our team focuses exclusively on venous health, making sure you receive the most current standard of care.
- Patient-Centered Approach: We don’t just treat the redness; we treat the person. We take the time to explain your ultrasound results and your long-term prognosis.
- Cutting-Edge Technology: We use the latest in non-invasive diagnostic and surgical tech to make sure your recovery is fast and your results are lasting.
Take the Next Step Toward Relief
Phlebitis is your body’s way of signaling that something is wrong with your circulation. Ignoring the pain won’t make the underlying cause go away, it only increases the risk of a more serious complication like DVT.
Don’t wait for a minor ache to become a major medical event. Contact Vanishing Veins today to book your consultation. Our experts will help you find the cause of your phlebitis and develop a plan to get you back on your feet, pain-free.