Navigating the world of medical insurance can feel like trying to find your way through a thick fog without a map. In our previous Insurance 101 installment, we touched upon the fundamental difference between insurance benefits and actual coverage, with a heavy focus on the “D-word”: Deductibles. As a quick refresher, your deductible is the specific amount of money you must pay out of pocket before your insurance company begins to contribute a single dime. This amount isn’t arbitrary; it is the contract you signed when you chose your specific health plan.
However, after decades of fighting the good fight against insurance companies on behalf of our patients, I must emphasize one golden rule: Benefits are not a guarantee of payment. Benefits mean that if you jump through every single hoop mandated by the insurer, you are eligible for coverage. Payment is never guaranteed, it is always buried in the fine print.
At Vanishing Veins, we believe that when you are in pain, you shouldn’t have to be an insurance expert. That is our job. Led by Dr. Lori Greenwald, a board-certified vascular surgeon and one of “America’s Top Surgeons”, our team is dedicated to helping you secure the benefits you pay for every month.
The Big Question: “How Soon Can I Get Treated?”
Once you’ve had your initial consultation and we’ve determined that you are suffering from venous insufficiency, the most common question we hear is: “When can we start?”
It is a natural question. If your legs ache, throb, or feel like they weigh a hundred pounds, you want relief yesterday. However, the path from “Consultation” to “Procedure” is paved with insurance mandates. To get your treatment authorized (meaning the insurance company agrees to pay), we must first prove “medical necessity.”
The “Trial of Conservative Management”: A Necessary Evil
Before we can even submit a request for a procedure like Radiofrequency Ablation (RFA) or Closure™, almost every insurance company requires a “Trial of Conservative Management.”
Think of this as the insurance company’s way of asking: “Can we fix this problem without paying for a surgery?” Depending on your specific policy, this trial typically lasts between 6 to 12 weeks. During this period, you are required to document that you have tried the following non-surgical interventions:
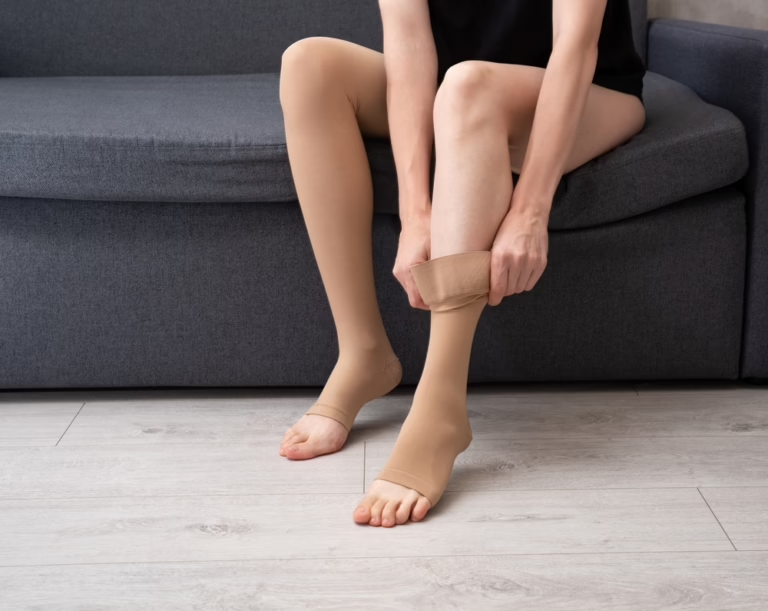
- Medical-Grade Compression Hose: These aren’t your grandmother’s stockings. These are specialized garments that apply graduated pressure to help your valves function.
- Leg Elevation: Propping your feet up above the level of your heart for at least 15–30 minutes, several times a day.
- Exercise & Weight Management: Walking or calf-strengthening exercises to engage the “muscle pump” in your legs.
- Anti-Inflammatory Medication: Utilizing NSAIDs (like Advil or Motrin) to manage the discomfort.
Why It Feels Like a “Run Around”
We understand that this feels like a waste of time. If your valves are fundamentally broken, a pair of stockings isn’t going to “cure” them; it’s just a temporary bandage. However, skipping this step guarantees a denial. At Vanishing Veins, we turn this “run around” into a streamlined process. Our vein specialists in New Britain can fit you for medical-grade compression hose right in our office, making sure you have the correct equipment to satisfy the insurance company’s requirements from day one.
The Vanishing Veins Clinical Protocol
While you are completing your conservative management trial, our clinical team is hard at work. We don’t just wait for the clock to run out; we use this time to build a “bulletproof” case for your coverage.
Our Diagnostic Expertise
Every successful insurance claim begins with a high-quality diagnostic ultrasound. At Vanishing Veins, our ultrasounds are performed by vein specialists in Glastonbury who understand the nuances of venous reflux. We document the exact diameter of the diseased veins and the duration of the blood “leaking” backward (measured in milliseconds).
This data is crucial. If an ultrasound is done poorly, or if it’s “faked” by having the patient lie down (as we discussed in our previous blog), insurance will reject the claim immediately. Our precision is your protection.
Advanced Treatment Options
Once we obtain authorization, we offer a suite of services designed for rapid recovery and high success rates:
- Radiofrequency Ablation (RFA): A minimally invasive heat treatment that closes the diseased vein.
- VenaSeal™: A proprietary medical adhesive that closes the vein without the need for multiple numbing injections.
- Microphlebectomy: A procedure where bulging surface veins are removed through tiny, “stitch-less” incisions.
- Sclerotherapy: Used primarily for smaller varicose and spider veins to make sure your legs not only feel better but look better too.
The Timeline: From First Visit to Surgery Day
To help you manage your expectations, here is the realistic timeline we follow at Vanishing Veins:
- Initial Consultation & Ultrasound: (Week 0) We identify the problem and establish the plan.
- Conservative Management Trial: (Weeks 1–12) You wear the hose and we document your symptoms.
- Follow-up Visit: (After the trial) We confirm that conservative measures weren’t enough to solve the problem.
- Prior Authorization Submission: (The same day as your follow-up) Our insurance experts submit your documentation.
- The Waiting Period: (Average of 4 weeks) This is the time it takes for the insurance company to review the files and issue an approval.
- Procedure Day: Once approved, we get you on the schedule immediately!
Exclusions: What if My Policy Doesn’t Have Benefits?
Sometimes, despite our best efforts, we discover an “Exclusion.” This means that your employer or the insurance company has specifically opted out of providing benefits for vein treatments, regardless of whether they are medically necessary.
This is frustrating, but it doesn’t mean you are without options. Even if your policy excludes the procedure, your consultation and ultrasound are usually still covered as a medical necessity to rule out dangerous conditions like Deep Vein Thrombosis (DVT) or blood clots. If you find yourself with an exclusion, Alethea and our finance team can discuss self-pay options and payment plans to make sure you don’t have to live in pain.
The Vanishing Veins Difference: We “Go to Bat” for You
The healthcare industry is changing, but our commitment to patient advocacy remains the same. Dr. Greenwald and her staff are experienced veterans in this field. We know the majority of the policies inside and out. If we encounter a new policy guideline we haven’t seen before, we don’t guess; we call the company directly on your behalf.
We are not a “vein mill.” We are a specialized vascular center that values the “Touch of a Woman and the Expertise of a Surgeon.” We want to make sure you get the insurance benefits you are paying for every month. Contact Vanishing Veins to schedule a consultation today.
This post was updated 2/19/26.