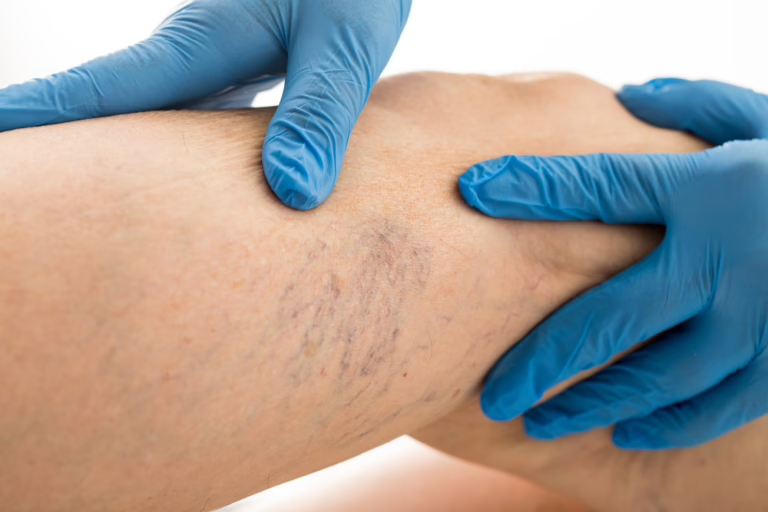
Pregnancy is a time of profound physical transformation. While many women are prepared for morning sickness or swollen ankles, they are often surprised and distressed by the appearance of vulvar varicosities. These are varicose veins (twisted, enlarged, and engorged) that develop on the outer female genitalia (the vulva).
If you are experiencing this, you are not alone. It is estimated that up to 10% to 20% of pregnant women develop these veins. Because the location is so intimate, many women feel a sense of embarrassment or hesitation to bring it up to their healthcare provider. However, understanding the physiology behind these veins can help demystify the condition and provide much-needed peace of mind.
Why Do Vulvar Varicosities Occur?
The human body undergoes a massive “vascular overhaul” during pregnancy to support the growing fetus. Several factors converge to create the perfect environment for vulvar varicosities:
1. Increased Blood Volume and Pelvic Flow
To provide nutrients to the baby, a woman’s total blood volume increases by nearly 50%. Much of this additional blood is directed toward the pelvic region. The veins, which are responsible for returning this blood to the heart, must work overtime to handle the increased load.
2. Hormonal Relaxation of Vein Walls
During pregnancy, the body produces high levels of progesterone. While this hormone is essential for maintaining the pregnancy, it has a side effect: it relaxes the smooth muscle in the walls of the veins. This makes the veins more “stretchy” and prone to dilating under pressure.
3. Mechanical Pressure from the Uterus
As the baby grows, the uterus becomes heavy and begins to press against the large veins in the pelvis, particularly the inferior vena cava. This creates a “back-up” of blood (venous hypertension) that flows into the smaller veins of the legs and the vulva.
Recognizing the Symptoms: Beyond the Visible
For many women, the first sign of vulvar varicosities is the appearance of blue, rope-like, or bulging veins in the genital area. However, the physical sensations can be just as significant as the visual changes.
Common symptoms include:
- Pressure and Fullness: A persistent “heavy” feeling in the pelvic floor, often described as if something is pushing downward.
- Localized Pain: Tenderness and soreness that may feel like a deep bruise.
- Exacerbation by Activity: Pain that intensifies after standing for long periods, physical exercise, or sexual activity.
- Perineal Involvement: The swelling can extend to the perineum (the area between the vagina and the anus) and is often associated with the development of hemorrhoids, which are essentially varicose veins of the rectum.
The Good News: Prognosis and Delivery
The most important thing for expecting mothers to know is that vulvar varicosities will not affect your pregnancy or your delivery.
Many women fear that these engorged veins will rupture or cause excessive bleeding during a vaginal birth. However, these veins have a very low pressure and generally collapse during the birthing process. They are not a reason to avoid a natural delivery or to opt for a C-section.
The Postpartum “Disappearing Act”
In the vast majority of cases, these veins will resolve on their own once the baby is born. As your blood volume returns to normal and the pressure on your pelvic veins is lifted, the varicosities usually shrink and disappear within six to eight weeks postpartum.
Management and Relief Strategies
While there is no “cure” for these veins during pregnancy (since the underlying cause, the baby, is still present), our vein doctor in Springfield recommends several ways to manage the discomfort:
Daily Lifestyle Adjustments
- Position Changes: Avoid sitting or standing in one place for too long. If you must stand, shift your weight frequently.
- Elevate the Hips: When resting, place a pillow under your hips to help gravity move blood out of the pelvic region.
- Left-Side Sleeping: Sleeping on your left side helps take the weight of the uterus off the inferior vena cava, improving overall circulation.
- Footwear Matters: Avoid high heels. They disrupt the “calf muscle pump” and can increase pressure in the lower body.
Physical Comfort Techniques
- Cold Compresses: Applying ice packs to the area can help reduce swelling and numb the soreness.
- Hydration: Drinking plenty of water helps maintain healthy blood viscosity.
- Compression Support: Specialized pregnancy support garments or pelvic floor support belts can provide “counter-pressure” that keeps the veins from engorging.
When to See a Specialist at Vanishing Veins
If your vulvar varicosities do not disappear within two months after delivery, it is time to consult a vein specialist in South Windsor. Persistent vulvar veins can sometimes be a sign of Pelvic Congestion Syndrome (PCS), where the internal veins of the ovaries and pelvis remain dilated and painful.
At Vanishing Veins, we provide a safe, professional, and discreet environment to discuss these intimate vascular issues. Led by Dr. Lori Greenwald, a board-certified vascular surgeon and Diplomate of the American Board of Venous and Lymphatic Medicine, our team offers the specialized expertise needed to treat postpartum vein issues.
Our Specialized Services Include:
- Advanced Pelvic Ultrasound: To check for “leaking” valves in the pelvic and ovarian veins.
- Vascular Mapping: Identifying if leg varicosities are being “fed” by persistent pelvic veins.
- Minimally Invasive Treatments: If the veins do not resolve, we offer modern solutions like sclerotherapy or embolization to close the problematic vessels permanently.
Why Dr. Lori Greenwald?
Dr. Greenwald has treated over 17,000 patients since 2003. She understands that vascular health is deeply personal. Her expertise as a vascular surgeon allows her to differentiate between normal pregnancy changes and underlying vascular conditions that require medical intervention. At Vanishing Veins, you aren’t just a patient; you are a woman receiving care from a specialist who understands the unique challenges of the female body.
Take the Next Step Toward Comfort
Vulvar varicosities are a common, albeit uncomfortable, part of the pregnancy journey for many. While they are usually temporary, the discomfort is very real. You don’t have to suffer in silence or feel embarrassed about the changes your body is experiencing.
If you are concerned about your veins during pregnancy, or if you are postpartum and your veins haven’t disappeared, give us a call. We are here to provide the reassurance, diagnosis, and treatment you need to feel like yourself again.
Contact Vanishing Veins to schedule an evaluation with Dr. Lori Greenwald. Let us help you navigate your vascular health with confidence.
This post was updated 2/18/26.